Pancreatic cancer numbers are growing, but treatments and diagnosis are also improving thanks to the work of researchers. Examples include the creation of a ‘phantom pancreas‘, the study of new markers predicting the efficacy of therapies and the use of Artificial Intelligence to predict post-operative complications. This is what doctors in Humanitas Research Hospital’s Pancreas Unit have been working on, besides taking care of over 1,000 patients affected by this disease every year.
“Darkness. When receiving the diagnosis of pancreatic cancer, it is as if the light goes out”. This thought is common to many patients affected by this type of cancer. Pancreatic cancer remains one of the big killers in oncology, with numbers on the rise: in Italy, cases have risen from 12,500 in 2015 to 14,300 in 2020, mostly amongst men between 65 and 69 and women between 75 and 79. Although the prognosis is often inauspicious, it has improved significantly compared to 10 years ago, but much scientific research still needs to be done to make diagnosis earlier and treatment more effective, as well as to raise awareness of this neoplasm’s symptoms.
The increase in pancreatic cancer numbers has several causes: unhealthy lifestyle, unbalanced diet and exposure to pollutants, first and foremost smoking, and lastly a genetic component in 10% of the cases (due to the mutated gene for BRCA or other rarer genes). Although some of these genetic predispositions are known, the absence of predictive or specific markers as well as clearly recognisable symptoms delay the diagnosis. This is why pancreatic cancer is rated 4th for mortality rate and could become the 2nd leading cause of death in Western countries within the next decade.
Prof. Alessandro Zerbi Head of Pancreatic Surgery at the IRCCS Istituto Clinico Humanitas and lecturer at Humanitas University, explains: “What makes the treatment of this neoplasm difficult is the deep anatomical position of the pancreas, its proximity to large veins and arteries, the poor responsiveness to treatment (always multimodal with chemo, surgery, if possible, and possible radiotherapy) and the often delayed diagnosis, which precludes the possibility of intervention, except in about 20-30% of cases. Hence the importance of stepping up research in innovative areas, both in terms of the mechanisms at the origin of the disease – which will allow us to develop new therapies – and the use of innovative approaches to improve surgical techniques’.
A ‘phantom pancreas’ to improve surgery and surgeon preparation
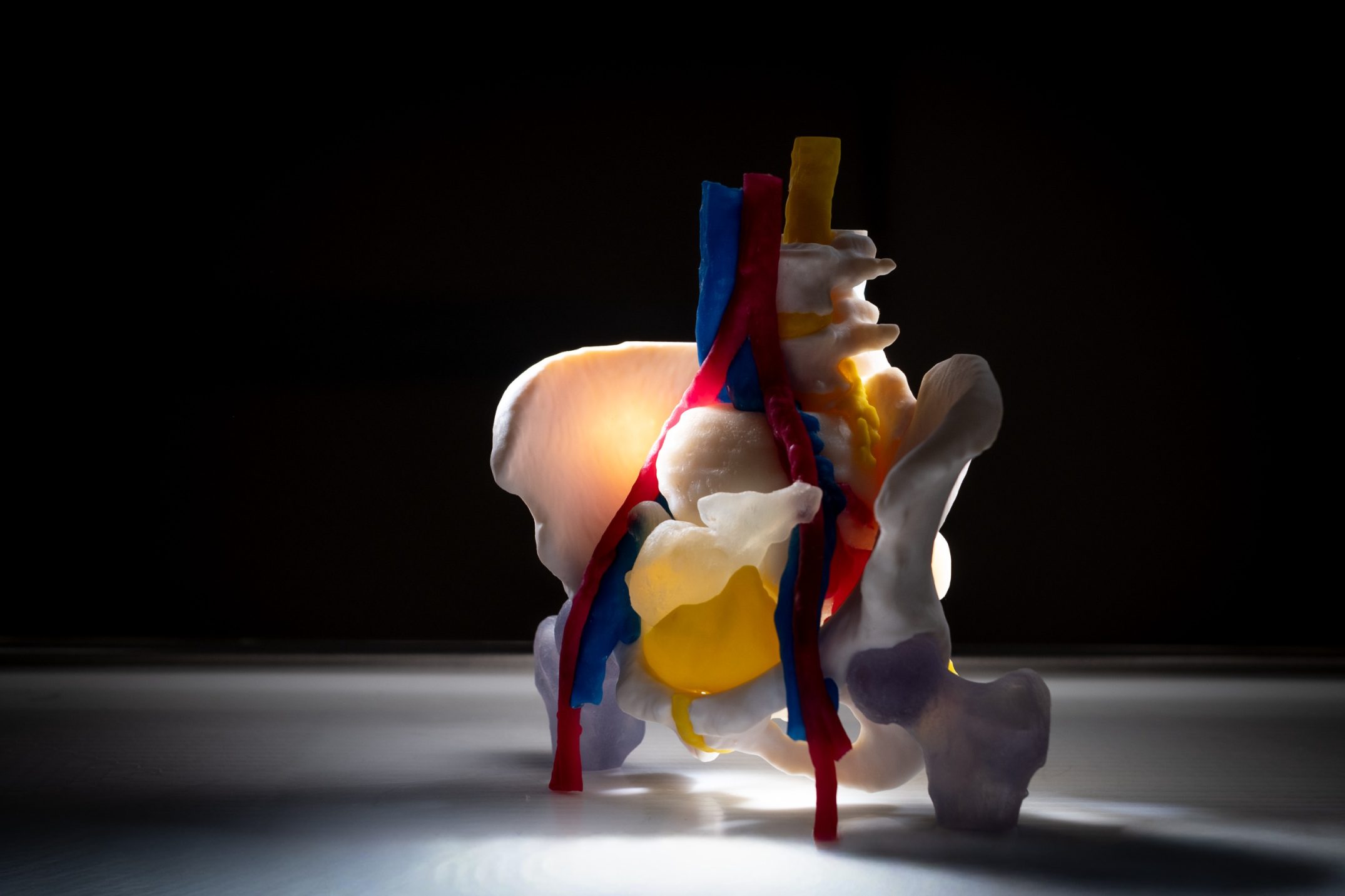
A collaboration between Humanitas University, IRCCS Istituto Clinico Humanitas and the Politecnico di Milano has led to the creation of a laboratory for the biomechanical and functional characterisation of pancreas tissue. The aim is to create a physical model of the organ (known as a ‘phantom’) made of artificial material, to train surgeons and residents but also to investigate specific instruments for pancreatic surgery, such as glues and suture threads with special characteristics.
“The research laboratory was developed in response to the need of professionals in the operating theatre: pancreatic surgery is in fact one of the most complex types, both because of where it is located and because of the characteristics of the organ, whose tissues are particularly fragile and delicate,’ comments Prof. Zerbi. ‘Moreover, very often the instruments and materials used for pancreatic surgery are not specifically designed for the pancreas, but are conceived for other organs and then adapted for this use case. However, each organ has specific anatomical and functional characteristics and the pancreas, in particular, is responsible for the production of pancreatic juice, which is very corrosive and can erode sutures after surgery, with the risk of haemorrhage or infection’.
‘Thanks to a special machine, it is possible to study small portions of pancreatic tissue and identify certain characteristics such as elastic modulus and mechanical resistance, upon which we can develop its complete characterisation,’ emphasises Prof. Maria Laura Costantino President of the MEDTEC School. This way, it will be possible to identify innovative and specific materials to be used in pancreas surgery, but also to develop a model in polymeric material that reproduces exactly its shape as well as its tactile, elastic and resistance characteristics, so that the surgeon can treat the organ even outside the operating theatre. An important step forward’.
Artificial Intelligence and Machine Learning to predict post-operative complications
Pancreatic cancer, although on the rise, is relatively uncommon. This makes it even more important to invest in artificial intelligence and the potential it offers in extracting useful information even from relatively small patient cohorts. This is the focus of a study funded by the Humanitas Foundation for Research’s 5×1000 and carried out with the support of the data scientists from the Humanitas AI Center.
“Our goal is to improve our ability to make pre-operative predictions and be able to assess, at an individual patient level, the likelihood of occurring complications as well as their severity, and lastly to implement limiting measures. To do this, we apply artificial intelligence algorithms to clinical data and preoperative imaging examinations, such as computed tomography. – explains Dr. Giovanni Capretti researcher and general surgeon specialising in pancreatic-duodenal pathology at the IRCCS Istituto Clinico Humanitas. The use of AI will, in the future, allow us to optimise the patient’s diagnosis and treatment, by potentially using only radio or chemotherapy treatment instead of surgery”.
Diagnosis and personalised medicine. Tumour profiling studies and predictive markers of therapy response
“In Humanitas,” adds Federica Marchesi, professor of general pathology at the University of Milan and researcher in the laboratories of IRCCS Istituto Clinico Humanitas, “we are involved in several research projects focused on identifying prognostic markers, especially metabolic and immunological ones: these are molecules, identified in tumour samples taken with a biopsy, that allow us to predict in advance, patient by patient, the response to a therapy. To identify them, we analyse both the tumour tissue and the microenvironment in which the tumour proliferates, including the cells of the immune system, through sophisticated multidimensional techniques’.
The role of fibrosis in pancreatic cancer
Another research project is the one focusing on the role of fibrosis in pancreatic cancer and born from the translational collaboration between pancreatic surgeons and researchers from the laboratories of IRCCS Istituto Clinico Humanitas. The term fibrosis refers to the thickening of tissue and the continuous formation of scars, and is caused by the immune activation and inflammatory state that is typical of a tumour. This phenomenon is particularly pronounced in pancreatic cancer, due to the characteristics of this organ, and its role in disease progression is still poorly understood. The project is being carried out by Prof. Zerbi’s team together with Sara Lovisa, a fibrosis expert who has returned to Italy from the MD Anderson Cancer Center in Houston thanks to AIRC Foundation’s ‘Start-Up’ grant, through which she is setting up her independent laboratory at IRCCS Istituto Clinico Humanitas.
Fighting resistant bacterial infections to improve prognosis of pancreatic surgeries
Improving the prognosis of pancreas surgery also means fighting possible bacterial infections which can be particularly dangerous due to the growing phenomenon of antibiotic resistance. Prior to removal of the pancreatic tumour, in fact, some patients must undergo endoscopic surgery to apply biliary stents, which are necessary to keep the bile ducts, obstructed by the tumour, open and functioning. However, it can happen that bacteria, mainly from the intestine, adhere to the surface of the stent and produce the so-called ‘biofim’, a protective layer that inhibits the action of antibiotics and hampers the immune system, facilitating the development of resistant infections. An interdisciplinary collaboration between surgeons and the research group of Prof. Roberto Rusconi Head of the applied physics, biophysics and microfluidics laboratory at IRCCS Istituto Clinico Humanitas, is using mathematical models and microfluidic devices to study the mechanisms of bacterial adhesion to the stent in order to prevent the biofilm formation.
Autotransplantation of pancreatic islets to reduce complications arising from complex surgeries
A team of researchers from the San Raffaele Diabetes Research Institute and surgeons from the Pancreas Center of IRCCS Ospedale San Raffaele and IRCCS Istituto Clinico Humanitas recently signed an important study in Annals of Surgery. The research shows that it is possible to reduce the complications arising from some particularly complex pancreatic surgeries by completely removing the pancreas and using, at the same time, the technique of the autologous transplantation of the patient’s pancreatic islets. This allows to preserve the production of pancreatic hormones, insulin and glucagon, which are necessary to regulate blood glucose control. (see dedicated press release: http://bit.ly/3h8GiU7)
The Pancreas Unit at Humanitas
The Cancer Centre of Humanitas has a Pancreas Unit that follows patients with pancreatic cancer and benign pathologies in a multidisciplinary way, carrying out basic and clinical studies also in collaboration with the Humanitas Foundation for Research.
The team includes oncologists, surgeons, radiotherapists, radiologists, echo-endoscopists, endocrinologists, pathologists and specialist nurses. Every year, more than 1,000 patients with pancreatic cancer are referred to the hospital, as well as approximately 250 cases of neuroendocrine tumours.